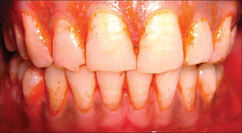
 For years, my relationship with chlorhexidine has been strained. The warning signs were there the entire time, so I should have known. You claimed to be able to assist me, yet all you managed to do was make things worse. I detest chlorhexidine. I have always detested the way you discolor the teeth I cherish so much and I found it infuriating that you would add calculus after I had spent so much time getting rid of it all. When I learned that you inhibit fibroblasts and have really killed patients, I was no longer willing to accept that everything had been done because you killed bacteria more effectively than the competition. There are numerous reasons why this relationship must end; dysfunction like this cannot be normal. 1- You only wanted a short term fling. I was so eager to introduce you to my patients when we first met. I was eager for them to test you out since I believed you could truly make a difference. I allowed you to assist me with those who needed it the most because I had been taught that you could be utilized for bleeding. Some of them had painful dental surgery, some had failing implants, and yet others had periodontal disease. I didn't realize you were really only meant to be used for gingivitis until much later. I believed you to be the best, and I kept trying to make it work, but you lied to me. However, because you need to be at such a high concentration (1200 ppm) to work, you are actually too harmful to use for more than two weeks. I want something that will last longer. 2- Do you even have a job? I started hearing a lot of bad things about you soon after we started dating. I eventually discovered that you really don't have the skills that I require to make this work. You fully tricked me into thinking you were excellent at all of these things, and I was stupid enough to fall for it. Now I'm hearing from other hygienists that you can't work in blood and saliva. Did you really think that the longer we were together, the less I would notice how ineffective you were? I can't believe you've been deceiving us all for so long. How could we ever make this work in the mouth if blood and saliva restrict you? 3- You’re literally toxic. Truly, utilizing you makes me feel awful, and I'm no longer able to ignore the fact that you treat my patients so poorly. After receiving dental care, they require a great deal of assistance to mend properly, and you are cytotoxic to the cells that support tissue regrowth. You cannot assist me in achieving my objectives for patient care while impairing the cells necessary for effective healing. I understand that I am contributing to this issue, so I have to quit. I will continue to make my job more difficult and inconvenience my cherished patients if I continue to offer you a choice. 4- You’re abusive. You did a wonderful job of keeping this small detail a secret, but after some discussion among the hygienists, your secret is now known. We are aware of her. The woman who passed away after utilizing you had just had her teeth pulled. I've also seen the FDA report on all the other serious allergic responses you've brought on. I'll never understand why you aren't completely prohibited from use, but I can't support you when you cause harm to others. I'm finally moving on. I've spent a lot of time improving myself and have accrued enough credits for continuing education to be aware that there are other, preferable possibilities. Activated chlorine dioxide is already my new passion. It not only kills bacteria more quickly, but it also eliminates viruses and fungi. It also decreases volatile sulfur compounds and helps me regulate biofilm without displaying any hazardous characteristics, and my patients adore it. I really hope no hygienist ever uses you again. Goodbye.
0 Comments
Since the early 1900s, oral rinsing has become a standard part of American culture. Consider for a moment that we are discussing a time when the typical household had an annual income of $3,000, no cars, phones, or indoor plumbing. And yet, mouth rinsing is still a cornerstone of general healthcare more than a century later. Today's options, however, are not the mouthwashes your grandfather used! Oral rinsing has undergone nothing short of a revolution, largely due to cutting-edge technologies and consumer demand. There is a seemingly endless supply of trendy flavors to persuade customers to buy and stay compliant, and new product compositions and iterations of old goods are routinely tried.
The repackaging of old goods and the emergence of novel, occasionally bizarre habits like oil pulling have caused dental practitioners all around the world to look into the most recent clinical studies. With claims of having analgesic, anti-inflammatory, antisepsis, and anti-cavity qualities, contemporary oral rinses are now frequently multifunctional treatments that are essential for preserving the patient's oral health. However, as we'll go over in more detail below, we are now also acknowledging the significance of mouth rinses in maintaining the safety of the dental hygienist while delivering clinical care. In addition to regular brushing, dental hygienists already know that oral rinse is one of the most adherent home care regimens we can suggest to our patients. We are aware of how crucial it is to cater our professional advice to every single patient based on their unique demands, behavioral traits, and health routines. Oral rinses can differ from one another just as much as the sun differs from the moon. Oral rinses can be acquired without a prescription, over the counter, or solely at dental offices, depending on the active ingredients. Oral rinses may be categorized as a medication, cosmetic, or both under the Federal Food, Drug and Cosmetic Act, depending on their intended usage. In order to determine the most common methods dental professionals are now using for oral rinses in a post-COVID-19 context, an informal survey of the American dental sector was conducted in October 2020. Unsurprisingly, using oral rinse as a pre-procedural rinse before the clinical session was by far the most common technique throughout the pandemic era. The cause? It is well established that pre-procedural rinsing greatly reduces oral bacteria. Activated chlorine dioxide, which is present in OraCare Health Rinse, is also useful against human coronavirus, according to an interesting new study published on July 1, 2020. In just one minute, the human coronavirus was found to be reduced by 99.99% by the activated chlorine dioxide in OraCare, and the reduction persisted for 60 minutes. These findings suggest that OraCare is an excellent pre-procedural rinse because it not only reduces the number of germs in the oral cavity but also might contribute to reducing the number of pathogenic microbes that are left over. Clinical technologies have advanced far beyond their 20th century roots, and cutting-edge oral rinses are currently being developed that can assist in treating several ailments at once. Take Jane Tooth, a pseudonymous 52-year-old Caucasian woman who struggles with obesity and a high-carbohydrate diet, as an example. In addition to not flossing, having a family history of heart disease, and having recently complained of dry mouth, Jane presents with a history of periodontal disease. She claims that she dislikes getting close to people because she feels self-conscious about her foul breath. Every three months, Jane sees her dental hygienist for periodontal maintenance. She is overdue for a thorough oral examination, full-mouth radiographic imaging, and periodontal charting. Oral rinse should continue to be an important part of Jane's home care routine as well as her professional appointments. The dental hygienist should employ an oral rinse during the clinical session as a pre-procedural rinse or as a post-procedural irrigation after rendering therapeutic care. Naturally, the dental hygienist needs to advise daily home rinsing as well. In this situation, a rinse that reduces oral odor can be selected, which will probably increase Jane's compliance. Future development of multipurpose oral rinses for the 21st century will make it more crucial than ever for formulations to reduce or eliminate negative side effects. Many more recent rinses, like chlorhexidine, have a reputation for staining, changing taste, and even causing oral discomfort, whereas older staple rinses like iodine and hydrogen peroxide claim a variety of negative effects. Since there was no cell toxicity at 60 minutes in the aforementioned study, activated chlorine dioxide found in Oracare is thankfully safe for human tissue. This makes activated chlorine dioxide completely safe for use on humans. It's critical to figure out how dental hygienists can keep using oral rinses in our clinical care as long as they remain common home items. It's similarly crucial to keep advising oral rinses to our patients as a supplement to brushing and interdental cleaning for at-home care. What an improvement for oral rinsing! 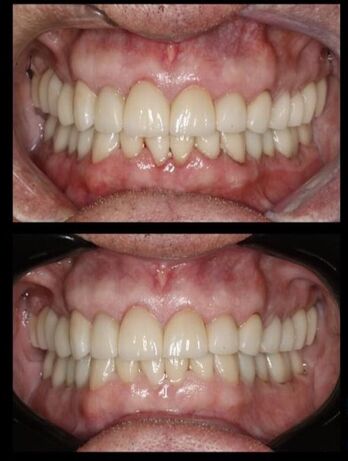 Pre-rinsing has become crucial as dental clinics around the nation consider what procedures to take to reopen after the pandemic. Numerous studies have shown that pre-rinsing can eliminate oral microorganisms before they are included in dental aerosols. In addition to bacteria, viruses, and fungi must also be destroyed by a pre-rinse. Activated chlorine dioxide (used in OraCare) is one of the few substances that can accomplish this safely. Let's examine activated chlorine dioxide in more detail. Activated Chlorine Dioxide (ClO2) Although it is more recent in dentistry, activated chlorine dioxide has been used for nearly 200 years to aid in disinfection in other industries. ClO2's adaptability as a disinfectant is ideal for any industry, including textiles, medicine, wastewater treatment, public health, food safety, and domestic usage. Because it is efficient against spore-forming bacteria, it has even been used to treat anthrax. Gaseous chlorine dioxide is a potent oxidant. It efficiently eliminates harmful microorganisms like bacteria, fungus, and viruses. Additionally, it stops and gets rid of biofilm. It can be strong enough to sterilize medical equipment while also being gentle enough to be administered intravenously to combat oral bacteria. ClO2 can be triggered in tiny or large amounts and at different intensities. It's crucial to understand that when the power increases, a material with a high oxidation potential reacts with more compounds. Chlorine dioxide has a strong oxidation power, but it is also low enough to prevent it from interacting with things that we do not want it to. Chlorine dioxide is a highly selective oxidant. This is why it is so perfect at eliminating oral bacteria while having no negative effects on our cells. Ozone and peroxide, however, are less selective in what they break down. Chlorine dioxide also has the advantage of being more efficient than some higher power oxidants (ozone and peroxide) at disinfecting a given volume of water or saliva. The rationale behind this is that a molecule like ozone, for instance, will interact with a lot of other salivary components and become exhausted before it has a chance to interact with the pathogen. This is why lower power ozone is preferable to chlorine dioxide in many situations, including water treatment. The bacteria and volatile sulfur compounds are the only organic molecules that the chlorine dioxide reacts with; other organic compounds that don't need to be treated are ignored. Therefore, even though a substance with a high potential strength would theoretically kill at lower doses, in practice it needs higher concentrations than chlorine dioxide to complete the job. ClO2 is ideally suited for utilization due in part to its strong oxidation capacities. In comparison to peroxide or ozone, it can oxidize 2.5 times more molecules. The oxidation capacity of chlorine dioxide is 5e, which means it can receive 5 electrons from the molecule it is oxidizing. Chlorine dioxide has an oxidation capability that is 2.5 times larger than that of hydrogen peroxide and ozone since they are only able to receive two electrons from the molecule they are oxidizing. Simply put, it removes more than twice as many electrons. But there are two steps involved in how this occurs. The first effect of the reaction is the reduction of sodium chlorite from chlorine dioxide. The sodium chlorite is then converted to sodium chloride, which is everyday table salt and water. The material has a chlorine molecule all the way to the end. This explains why trihalomethanes and other hazardous chlorinated compounds are not produced by chlorine dioxide. Some people mistake chlorine dioxide for chlorine bleach. They differ not just in structure but also in behavior; therefore, it is not chlorine bleach. Compared to regular chlorine bleach, chlorine dioxide is an extremely selective oxidant. The cell wall of bacteria is pierced during chlorine dioxide eradication. Chlorine dioxide reacts with bacterial cells, disrupting a number of cellular functions. Amino acids and RNA in the cell are immediately reacting with chlorine dioxide. It is unclear whether chlorine dioxide damages the internal cell acids or the cell structure, but it does stop the creation of proteins. By altering membrane proteins and lipids as well as by preventing inhalation, chlorine dioxide has an impact on cell membranes. ClO2 is at least as effective as chlorine as a bactericide, but oftentimes it is greater. In particular, its superiority as a virucide sets it apart from the competition. Chlorine Dioxide and Viruses In contrast to bacteria, viruses are destroyed by a reaction between chlorine dioxide and peptone, a water-soluble product of the hydrolysis of proteins into amino acids. Viruses are destroyed by chlorine dioxide by stopping the synthesis of proteins. "Neither chlorine nor ozone are more effective against viruses than chlorine dioxide." It functions well across a wide pH range due to its radical nature. Living cell walls appear to be more permeable to gaseous chlorine dioxide radicals, making it simpler for essential chemicals to enter. Even medical equipment and electronic devices utilized in the treatment of patients on the front lines of the fight against Ebola in West Africa were sterilized by the US military using chlorine dioxide. Additionally, it has a history of use and success against the influenza A virus. Know the Difference (Activated vs. Stabilized ClO2) There is one last, crucial thing to address before we wrap this up. This means that the terms "stabilized" or "naturally activated" chlorine dioxide are used to describe products. This is not accurate, and you do not receive all of the advantages of chlorine dioxide. In actuality, the substance referred to as "stabilized chlorine dioxide" or "naturally activated" is sodium chlorite (a salt). You need to combine an acid and a basic salt solution to create genuine chlorine dioxide, which is a gas. Gaseous chlorine dioxide is released as a result. Because of this, OraCare is available in a two-bottle system and needs to be mixed thoroughly before each use. While sodium chlorite still offers some advantages, they pale in comparison to those of activated chlorine dioxide, particularly the fact that it does not eradicate viruses. Chlorine Dioxide and Dentistry Finally, it is being used more frequently in dentistry. It's utilized for a lot more things than just replacing chlorhexidine, like implants, periodontal disease, bad breath, dry mouth, pre-rinsing, and post-op. Dental professionals have reached a new level as a result of its capacity to eliminate bacteria as effectively as chlorhexidine without causing any negative side effects and other advantages. As a pre-rinse every day in office, activated chlorine dioxide can protect us and meet all of our professional needs, especially in light of the current rise in virus-related anxiety. OraCare products contain activated chlorine dioxide, which is combined with xylitol. Only dentist offices sell OraCare Health Rinse. Dentistry has changed since 1954, so should your rinse. There is an alternative. For more information visit OraCareProducts.com or call 1-855-255-6722. The tongue is home to more than half of the oral germs, and patients frequently complain about having bad breath. But how frequently do dental hygienists talk to their patients about this important organ? I'd argue for an alternative way of thinking (and explains why using a toothbrush to brush the tongue is ineffective).
I recently ran a non-scientific "research" in which I posed the following queries to 20 healthy individuals: "During your most recent dentist visit, were you instructed on how to properly care for your tongue? Has someone brought up the bacteria that lives on your tongue? Did they mention your tongue in any way?” None of them could think of a time when their dentist or doctor had discussed regular tongue care with them. All of them had generally decent dental health. This begs the question: Do we even discuss the tongue at the appointment if the patient is healthy, has no coating on their tongue, and has no offensive odor coming from their mouth? I don't remember learning how to clean my tongue in oral hygiene class. Even so, I don't recall ever receiving a score for my ability to evaluate the tongue or to properly care for it. We are all aware that the area of the mouth in question is a breeding ground for germs that might cause further complications. Why aren't we talking more about how to take care of our tongues? We shouldn't ignore this responsibility that is placed on our shoulders as qualified dental hygienists, just as we do when caring for teeth and the surrounding tissues. There are a lot of patients who don't take care of this very substantial section of the mouth, even if my unscientific study is only partially accurate. This is why I call it "neglected duty." Why it needs to be addressed I am aware that "neglect" is a strong word and that we don’t ignore the tongue on purpose. But crucial information about a patient's general health can be gathered from their tongue. In addition, eating, breathing, speaking, and swallowing may be difficult if our tongues are not in good shape. It is simply time to learn some new techniques for taking care of this highly significant organ. We must be careful to pay attention to healthy tongues in general rather than just those with evident problems because the tongue can easily become unhealthy, much like teeth and gums. On the tongue are more than half the germs in the mouth. This may potentially exacerbate other problems. At the moment, when we discuss the tongue, we typically discuss foul breath. Many of us are aware of the link between the tongue and odor, but malodor's underlying causes result in problems beyond just poor breath. The odor is caused by the bacteria's emission of volatile sulfur compounds (VSCs), which are also associated with the development of gum disease and sluggish wound healing. The tongue is the area of the mouth where plaque builds up the most, making it the perfect place for germs to flourish. Starting the conversation There are two schools of thought on how to clean the tongue. The first is to either perform the action on behalf of the patient during the visit or let the patient perform the action on their own. You can clean your tongue however you please, but in order to make it a priority, we need to start talking about it during the appointment, just like we do with brushing and flossing. The intention is for patients to take care of their tongues daily at home. The past is the past, but because we now understand the value of tongue cleansing, we must inform our patients. Everybody should have a tongue scraper nearby, just like they do a piece of floss. Be sure to explain to patients that even though their tongues may seem clean right now, bacteria will repopulate, necessitating daily repetition of this procedure. Realistically, the entire mouth is affected by this. Patients should think of their cleanings as a new beginning on the road to better health. The Right Tools Some patients make an effort to take care of their tongues by brushing them with their toothbrush. This does little in the way of eradication and largely just pushes the bacteria and other germs on the tongue around. They might spread germs that cause additional problems if they clean their teeth with the same toothbrush. For this reason, a tongue scraper ought to be utilized both at home and at the office. Just as floss is used to clean the surfaces between teeth, a tongue scraper should be used to clean the tongue. Specialized areas demand unique equipment. When compared to simply brushing, scraping the tongue can eliminate 30% more bacteria. Furthermore, a tongue scraper does not exacerbate a bad gag reflex as much as a toothbrush does. The dorsal and lateral regions of the tongue, in particular, can be quite challenging for patients to access. Therefore, taking care of these delicate places will require more than just using a tongue scraper. Here's where picking a rinse becomes important. Rinses assist with both the tongue's unbrushed parts as well as the regions that brushing and flossing miss. For both a healthy mouth and fresh breath, choosing a rinse that removes the VSCs on the tongue is crucial. My Preference If you are now wondering, "What are the right tools to use to clean the tongue?" I have a few suggestions. For a couple reasons, I like the OraCare Tongue Sweep. First, I contributed to its design, so that undoubtedly has an impact. However, the main reason I would pick the Tongue Sweep over alternatives is that it was made to remove debris from the tongue quickly and easily. It comes in a three-pack with different colors, so it can be sufficient to cover a patient in between appointments or be enough for the whole family. The tongue scraper and OraCare Health Rinse, in my opinion, offer the best plaque removal and VSC eradication. This helps with foul breath, a common patient issue. OraCare offers a "30-day Bad Breath Challenge" to encourage patients to experiment with new routines. Talking about the entire mouth and not just the teeth is the most crucial lesson I want hygienists to learn from this article. Starting the discussion and eliminating the neglect can only improve our care as experts because the tongue is a significant component of the mouth that needs regular care. 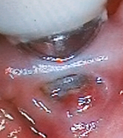 As implants become a more common option to replace natural teeth, so do their issues. The most common reason for implant failure is peri-implantitis, which is brought on by too much biofilm. Implant failure is on the rise. The only way to get rid of this biofilm is to work with patients to develop a simple at-home regimen. The issue is that implants are frequently inserted into the mouths of patients who most likely lost their original tooth (or teeth) as a result of years of neglecting their dental care. Poor home care is the root of most oral health problems, including implant failure. Even when the original tooth has been replaced, the condition persists. Long-term implant success depends on educating patients about the fact that failure of an implant occurs for the same reasons that their natural tooth failed. When a patient becomes a candidate for implant placement, dental practitioners need to provide them with the appropriate tools and knowledge. Let's look into strategies for controlling implants and the development of peri-implant illness. Before The Implant Is Placed Giving implants to people whose oral hygiene caused them to lose their natural teeth is the same as giving an alcoholic a new liver. Without reform, the issue is likely to stay the same. We may use the reasoning that many orthodontic offices employ before treatment, where the patient occasionally needs to "show" that they are able to maintain their oral hygiene. If not, therapy is put on hold until they can show improvement. Patient compliance impacts the success of an implant, much like it does in orthodontics. This point must be understood by the patient. Since we encourage patients with poor oral hygiene to refrain from brushing or flossing the surgical site for a few weeks while it heals, implants provide a unique set of challenges from the start.The poor habits that were already in place are just reinforced by this. One of the most crucial duties for a patient is the management of biofilm (dental plaque), which is necessary for the long-term effectiveness of an implant and the avoidance of peri-implantitis. According to numerous studies, the main etiological factor in the onset and spread of peri-implant infections is biofilm. The therapeutic properties of being able to break up biofilm or kill bacteria (and other pathogens) are not present in products like toothpaste, flossing, water piking, interdental brushes, etc. These are all mechanical techniques of removal. Biofilm, in particular around an implant, can be challenging to remove because it is difficult to reach with standard brushing and flossing. Therefore, a device that is both therapeutically effective and able to reach difficult-to-reach places must be used. Maintaining Implant Health There are several clinical therapies available to help manage peri-implant disorders, but the key to excellent outcomes is early detection and avoidance of problems. Infection, poor dental health, and general ill health are all factors that might cause implants to fail during the initial stages of installation. Thus, keeping the hard and soft tissues around the implant healthy is essential because they serve as biological barriers to prevent peri-implant illness. Periodontitis and peri-implant disease are both caused by microorganisms that are closely related to one another. These include microorganisms such as bacteria, viruses, fungi, and biofilm. The microorganisms are left behind in uncleaned, undisturbed parts of the mouth and, similar to periodontal disease, become more sophisticated as they age. This makes them more difficult to get rid of over time. This is why peri-mucositis is the first infection to show up surrounding a poorly maintained implant. In contrast to more severe, permanent peri-implantitis, this can be reversed. It is our responsibility as dental professionals to aid in the prevention of this condition and instruct patients on the appropriate instruments to use. Reducing The Risk For Implant Failure Consequently, how can we assist? During the healing process, implants need to be protected. In a perfect world, the defense would start during surgery, with therapeutic medicines helping to lessen pollutants at the surgical site. Since they cannot employ mechanical means of disruption during this period, they must instead continue to keep the area clean using something like a rinse. This will not only improve the environment for recovery but also highlight the need to provide their newest member with specialized care. A rinse might help with implant maintenance in the long run. We advise our patients to clean and floss their teeth, and we hope they do so frequently, but even when they do, it is still purely mechanical. If these measures were sufficient to prevent gum disease, just 47% of Americans would have it, and that percentage wouldn't rise to 70% after age 60. These numbers are bad news for dental implants because they are more difficult to maintain using conventional methods. In order to provide patients with implants, improved techniques for treatment must be adopted as quickly as possible. To reduce the risk of implant failure, a treatment alternative that eliminates bacteria, fungi, and viruses as well as neutralizes volatile sulfur compounds and disassembles biofilm is required. Studies have found that certain goods' medicinal ingredients can lessen the viability of pathogens in biofilm. Activated chlorine dioxide falls under this category. It has the power to eliminate fungi, viruses, bacteria, and biofilm while lowering volatile sulfur compounds. Daily usage of this active component for implants and general hygiene is safe. The Reassure system from OraCare is one such item that includes these components. Both a gel and a take-home rinse are included in this medication to assist the patient after surgery. It is our responsibility to develop more effective methods to prevent peri-implantitis given the rising popularity of implants. We need to give patients the right equipment because we are aware that most implant failures are caused by subpar homecare. Our best defense against the leading reason for implant failure is to develop a daily routine that includes a rinse with therapeutic benefits. We have all had in-depth discussions about brushing and flossing with patients. Although the recommended brushing duration is 4 minutes per day, most people make an effort to brush for 40 to 70 seconds on average each day. Some people floss, but none of my patients do (hopefully yours do). It is hardly surprising that 76% of American adults have gum disease in some form. But how can we reduce this figure? Although I don't believe that what we are doing now is incorrect, our strategy for preventing and treating gum disease needs to be changed. The mechanical actions of brushing and flossing don't actually kill anything but will physically remove plaque from teeth. These two conventional procedures don't help the body fight systemic oral infections, they don't kill bacteria, and they don't lower therapeutic volatile sulfur compounds, all of which play a part in gum disease. Let's examine each of the three approaches and how they might be used to combat this expanding issue.
Mechanical Mechanical removal techniques include brushing, flossing with string or water, and general interdental cleaning. Brushing and interdental cleaning are crucial, and there is no disputing that. These techniques are essential for better oral hygiene. The real meaning of mechanical removal, however, is "picking up germs and throwing them away, rather than killing them with chemicals or heat.” Simply removing some of the plaque from the tooth during brushing and flossing, adding it to our saliva along with some toothpaste (for fresh breath, of course), and then spitting it all out is brushing and flossing. It offers nothing to aid the patient in battling an ongoing infection and does nothing to eradicate any pathogenic germs. Brushing and flossing are not sufficient if our ultimate goal is to reduce gum disease in our patients. Systemic It is very challenging to control a disease once it has spread to the oral cavity. This is especially true in cases of periodontal disease, which gets worse over time if left untreated. Once the infection has been shown to be active, it can be treated with an antibiotic to start periodontal therapy. This is fantastic for treating the initial infection, but a patient cannot take antibiotics for an extended period of time. As your body develops resistance, using antibiotics may become ineffective in the future. We definitely do not want this to occur. We require an additional resource that our patients can regularly and securely use. Therapeutic The greatest features of mechanical and systemic removal are combined with therapeutic choices to improve routine treatment. The primary item that fits into this category are rinses. As a result of how simple a rinse is for patients to use, this is where we may have a tremendous impact on dental health. In addition to reducing viruses, fungus, and volatile sulfur compounds (VSCs), some rinses can also break up biofilm and kill bacteria, all of which are linked to gum disease and other oral illnesses. It is crucial to remember that not all rinses have these features or can be used for a prolonged period of time; thus, strict criteria should be utilized when selecting rinses. As an example, chlorhexidine is excellent at killing bacteria but ineffective against viruses, fungus, biofilm, or VSCs and has a short shelf life. In addition to its therapeutic limits, the buildup of stains and calculus adds to the workload. Better patient health is what we're after, not adding on more work. Activated chlorine dioxide is an active component to look for in rinses. The same germs that chlorhexidine and other disease-causing pathogens quickly destroy with this substance, but without the unpleasant side effects (no staining, yay!) and may be used for long-term daily use without risk. OraCare is a rinse made with activated chlorine dioxide that is sold in dental offices. The addition of xylitol to this rinse only increases its medicinal advantages. Additionally, patients will actually utilize it, and they’ll love the taste. Every day, mechanical and therapeutic measures must be used to combat gum disease, and if an infection is present, systemic treatment may also be necessary. In 1954, chlorhexidine was first used in clinical settings. Since then, patients have received it to treat a range of dental problems, including but not limited to gum irritation, swelling, and bleeding. Great, right? Wrong. While there are benefits to this rinsing, the disadvantages outweigh them by a wide margin. Which raises the question of whether we should continue using chlorhexidine. Let's explore this further to find the answer.
Dental offices now use chlorhexidine as a "safety shield." Even though it's solely meant to treat gingivitis, many dental practitioners advise using it for a number of off-label purposes. This rinse is recommended as a last resort. How effective is it, though? Even though chlorhexidine has excellent antibacterial properties and can treat gingivitis, it also contains a substantial amount of 1200 parts per million. This then raises the possibility of adverse side effects. Many people are not aware of the more serious repercussions, one of which is the inhibition of fibroblasts, even though the majority of chlorhexidine users report "manageable" side effects (i.e. staining). In a 1991 study, it was discovered that using 0.12% chlorhexidine on human gingival fibroblasts greatly hampered the periodontium's ability to heal and regenerate. The additional dangers associated with patients utilizing the rinse over an extended period of time are a serious issue as well. As briefly indicated above, this product has exceptionally high parts per million, which limits consumption to no more than two weeks. Unaware of the additional harm they are doing to both their patients and themselves, sadly, many dental professionals are sending their periodontal patients home with the product to use after this time period. Even though it may be unfortunate, these are not the only issues. Staining, burning, cytotoxicity, calculus formation, inactivation in blood/saliva, etc. are a few of the other contraindications. Why is it still suggested, then? Comfortability, to put it simply. 68 years ago, dental practitioners learned about chlorhexidine in academic settings, and it’s been carried over since. Consequently, it became their only alternative. But chlorhexidine is no longer considered the gold standard of care, just like other dental treatments, procedures, and products that were formerly advised. Let's examine amalgams as an example. 150 years later, we are learning that amalgams are poisonous, impair tooth structure, and can cause significant illness or additional decay. Don't forget about airflow versus scale and polish. This approach is not only quicker but also more effective because it can clean those difficult-to-reach areas. As is evident, dentistry has advanced. Because of the convenience of use, the technique, and the risks, we have subsequently progressed past the previously described. With chlorhexidine, it's time to take similar action. Despite the fact that chlorhexidine's dangers clearly exceed its benefits, many dental offices continue to use this rinse. This often comes down to familiarity and a lack of understanding about a better option. The good news is that activated chlorine dioxide is an additional choice. Although activated chlorine dioxide (CLO2) has been around since the 1800s, the dental industry only became aware of it in the early 2000s. While not to be mistaken with stabilized chlorine dioxide (NaCLO2), this potent ingredient treats a variety of dental problems, including halitosis and periodontitis. To enhance the oral health of all dental patients, it can be applied universally in dentistry. Additionally, it can address similar problems at considerably lower parts per million (44ppm). The best part of activated chlorine dioxide is that it has neither adverse effects nor limitations. As a result, this serves as both a chlorhexidine substitute and a general oral health option. In light of the findings, we no longer have to rely solely on believing in and trusting chlorhexidine. To answer the original query posed at the start of this article, "Should we still be using chlorhexidine?" The response is simple to understand. No.  We are all aware that there is a pandemic going on. Everyone has encountered deserted waiting areas, burning through multiple layers of PPE, and intensified disinfection efforts, but there may be some good news. We can see this as a chance to modernize our infection prevention measures, which is crucial for our patients, ourselves, and our families. You now have your doctor's attention; therefore, there is no time like the present. This pandemic is forcing us to alter our practices, much like the HIV/AIDS crisis did in the 1980s. Both the modifications we made at the time and the current modifications are required advancements. Previously, treating a patient without gloves was permissible, but today, that is the accepted standard of care. Pre-rinsing has always been advised but is only recently being acknowledged as an essential step in infection management, similar to the wearing of gloves. It is well known that dental aerosols are dangerous. Pre-rinsing, however, kills the bacteria before they become aerosolized, in contrast to the majority of our present PPE, which is made to act as a barrier between us and particles. Is this effective? Let's turn to science; a recent study found that pre-procedural rinse significantly reduces the germs in aerosols by 97%. This result was discovered by taping agar plates to the walls of a treatment room during the investigation. The plates were subsequently grown in an incubator following the aerosol exposure. There was 94% less bacterial growth when the patient pre-rinsed before receiving treatment. As a result, there will be less bacteria on the countertops, walls, equipment, air, operator's clothing, and clinician's lungs. This demonstrates that a little pre-rinse can at the very least cut down on the contaminants that are still in the air. Pre-rinsing is a straightforward process, but picking the ideal rinse can be challenging. While viruses are under scrutiny in the contemporary climate, bacteria have historically been the primary concern in dentistry. As a result, several commonly used pre-rinses (such as Listerine and Chlorhexidine) do relatively little to eliminate viruses. Pre-rinses have to be able to eradicate fungus and viruses in addition to bacteria. A good pre-rinse should also have the capacity to kill swiftly, ideally in under a minute. In a typical dental situation, waiting 5 to 10 minutes for your pre-rinse to take effect is not practical. Who has time to wait that long to begin treating their patient? For instance, hydrogen peroxide shows limited virucidal activity until 5 minutes of contact, and effectiveness also seems to decline with a decreased concentration of the active element. Additionally, effectiveness seems to decline with a decreased concentration of the active element. Using commercially available rinses (1.5% and 3.0% H2O2), a research by the American College of Prosthodontists found that these concentrations have limited virucidal action at both 15 and 30 second exposures, which is a normal rinse time. Few compounds rival the oxidizing potency of chlorine dioxide when it comes to destroying bacteria, fungus, and viruses. Chlorine dioxide has been used to aid in disinfection in various industries for close to 200 years, despite its more recent application in dentistry. In contrast to other oxidizers like ozone and peroxide, chlorine dioxide is a very selective oxidizer. What does the term "selective" mean? Ozone and peroxide are stronger oxidants that react with many of the other components of saliva because they are less selective in what they break down. The oxidation potential is exhausted before it has a chance to interact with the target pathogen. Additionally, it interacts with bodily cells, which has a detrimental effect on tissue responsiveness. For this reason, surgeons traditionally avoid using products that include peroxide. Chlorine dioxide is safe and efficient. Even medical equipment and electronic devices utilized in the treatment of patients on the front lines of the fight against Ebola in West Africa were sterilized by the US military using chlorine dioxide. Additionally, it has a history of use and success against the influenza A virus. OraCare is one of the only products that uses activated chlorine dioxide. It has various medical applications, but pre/post rinsing has been its primary use for the past ten years. Furthermore, a recent study validated OraCare's capacity to eradicate human Coronavirus with no cell damage. OraCare can safeguard you as a dental expert in addition to helping your patients' oral health. Learn about your options because there are many, as with anything else. Any pre-rinse is always preferable to doing nothing at all. Just make sure the rinse you select eliminates all the microorganisms without harming your patient. Things will change once we start treating patients like "normal" again. I can be assured of this. There might even be updated OSHA regulations, or we'll at least adhere to the existing regulations much more closely. Pre-rinsing is one aspect of every patient visit that will remain constant. Despite the fact that we were all taught to do this in school and that we should all be doing it, less than 20% of the people I contacted (I contacted 25 friends) pre-rinsed prior to the Covid-19 pandemic. If you're still not convinced, ask yourself if you pre-rinsed everyone. I predict that the answer is no, but I'm fairly confident that after the pandemic, that will be near 100%.
Why Pre-Rinse? Some of the most hazardous contaminant transmitters in the dental office are dental aerosols. During an appointment, secretions from the nose, throat, and blood can all get aerosolized. These aerosols, which contain bacteria, viruses, and fungus, can be inhaled more than once, land on surfaces, and persist in the air. According to studies, pollutants can spread approximately 30 feet and may even be found on surfaces that aren't being used at the time of a dental treatment. The amount of germs, viruses, and fungi that are expelled from the mouth as aerosols should be reduced or eliminated. Chlorhexidine or another widely accessible over-the-counter product has been utilized by many pre-rinsing offices; this is preferable to doing nothing. However, these medications are only effective against bacteria and have no effect on viruses or fungi. The decrease in viruses is essential to protecting ourselves and our patients, as recent occurrences have brought to our attention. You must find a pre-rinse that is efficient against each of these infections, particularly viruses, if you want to lower the danger. Few chemical substances can match the oxidizing strength of chlorine dioxide when it comes to killing bacteria, fungus, and viruses. It has a long history of use, is effective against bacteria, viruses, and fungi, and is applied to various industries to dissolve biofilm. Unexpectedly, it is a gas that water treatment plants have long employed to keep drinking water safe. In the aftermath of anthrax attacks, it has also been used to disinfect buildings and post-harvest food. Because chlorine dioxide has a distinct and superior method of eliminating bacteria compared to other disinfectants, it is used in each of these instances. As a virucide, it stands out in particular as being superior to many other products. Activated chlorine dioxide is often regarded as the perfect pre-rinse by dental practitioners. Many dental clinics now include it in their daily routine of personal preventive measures due to its efficiency in killing not only bacteria but also viruses and fungi. Stabilized chlorine dioxide is something to be on the lookout for. You might believe you are receiving all of these advantages when you are not, since this is not genuine chlorine dioxide. Unfortunately, the term "stabilized chlorine dioxide" is incorrectly used to refer to sodium chlorite, a salt, whereas in fact the compound is stabilized chlorine dioxide. The term "stabilized" seeks to designate a formulation with qualities chemically equivalent to or similar to activated chlorine dioxide. They are remarkably dissimilar. By buffering sodium chlorite with carbonate, phosphate, and hydrogen peroxide, stabilized chlorine dioxide is created. In actuality, this method stabilizes chlorite rather than chlorine dioxide. The stabilized substance differs from chlorine dioxide and does not possess the same oxidizing qualities. The chemical is substantially less effective as a product in general and has a much lower oxidizing potential. Since it would be difficult to hold the gas in a single bottle, genuine chlorine dioxide must be mixed every time before use. Activated chlorine dioxide is the gas that is produced when those two liquids combine. The active components in OraCare include xylitol and activated chlorine dioxide. Patients can use it for a variety of conditions, such as oral sores, dry mouth, foul breath, periodontitis, and bleeding gums. In-office usage includes irrigation and pre/post rinsing. OraCare can safeguard you as a dental professional in addition to assisting with oral health improvement. The moment has come to examine our daily defensive measures critically. In truth, we are always at risk, and pre-rinsing is a crucial step in ensuring our safety. At some point during our dentistry careers, we have all heard about Chlorhexidine. We were instructed to use it in office after being taught about it at school. It used to be the only option, but as dentistry changes, it's critical that we talk about the misconceptions and realities surrounding the rinse that experts in the field of dentistry so frequently advocate for and employ.
Here are five myths and the reasons why you should start looking for a substitute. Myth: Long-term CHX use is possible. Truth: It should only be used for two weeks at most. A two week time frame doesn't work because tissue needs at least 30 days to recover. For the duration of the healing process, patients will need to continually try to minimize the bacteria and volatile sulfur compounds that inhibit wound healing after a procedure. If used for more than two weeks, the patient's teeth will eventually become visibly stained and will develop further calculus, which can only be removed by a professional cleaning. The aftertaste is greatly disliked by many patients. Patients will have to wait for numerous hours for Chx to take effect, which creates a major barrier and is the reason for low compliance. Using Chx as a long-term alternative should be undesirable because of these adverse effects, the possibility of allergic responses, the inhibition of fibroblasts, and its subpar antibacterial properties. Myth: The only issue with CHX is that it causes dental discoloration. Truth: Patients and dental hygienists both complain about staining most frequently, and they both agree that it makes their jobs more challenging. However, it is not the only negative impact. One significant concern involves uncommon but unavoidable allergic reactions, which might present as minor mouth burning or extreme life-threatening symptoms. Chx inhibits fibroblasts, has subpar antibacterial properties, and recent research has discovered problems with Antimicrobial Resistance (AMR), where the rinse itself degrades and develops cross-resistance to other types of bacteria. Every time a patient uses Chx, staff and the patient should keep these more serious hazards in mind. Myth: Using Chx as a pre-rinse is adequate. Truth: Chx has weak antiviral properties. In reality, there is conflicting information regarding Chx's capacity to lessen oral microbial load. Studies on Chx's antiviral properties reveal that what it does kill occurs over a long period of time, preventing it from killing viruses quickly enough to be an effective pre-rinse. Can it be helpful if we use it to lower the microbial load before treating a patient but it takes many hours to do so? Isn't that the point behind the pre-rinse? Myth: You can use chx for perio, implants, and post-operative care. Truth: Chx should only be used to treat gingivitis. Chx is a powerful weapon against germs, according to research, but it also causes a high rate of cell death in human gingival fibroblasts and kills without discrimination. Chx has a strong potential for cytotoxicity, and since it needs fibroblasts for tissue repair, it slows down the healing process. To aid in healing during the crucial healing phase following an SRP or treatment, healthy cells and fibroblasts are required. Simply put, a salt rinse works better than a Chx rinse after surgery. Myth: Chlorhexidine is the only rinse that effectively destroys bacteria. Truth: Chx is not the only professional choice. Even with all of its drawbacks, we already know the truth about Chx: it is efficient against bacteria. But does it make sense to continue using it after taking all of the dangers and adverse effects into account? There is one rinse that is the only other choice. OraCare. When OraCare's active component, chlorine dioxide, is activated, it has the same effectiveness in killing bacteria as Chx while doing so with fewer parts per million. It has been determined to be the best replacement for Chx due to its capacity to eradicate viruses, fungus, and volatile sulfur compounds while posing no adverse side effects and improving home care. |
Kristin Goodfellow RDHKristin is Chief Clinical Officer of OraCare, a practicing Registered Dental Hygienist Archives
August 2023
Categories |
1-855-255-6722OraCare is made in the USA.
|
OraCare© COPYRIGHT 2015. ALL RIGHTS RESERVED.



 RSS Feed
RSS Feed